 Unfortunately, I had to neglect my blogs for some considerable time due to disease and pressure from my businesses. This has been very frustrating for me but I really had no choice, my work pays the bills and I had reached the point where I was working twelve to fourteen hours every day, including weekends.
Unfortunately, I had to neglect my blogs for some considerable time due to disease and pressure from my businesses. This has been very frustrating for me but I really had no choice, my work pays the bills and I had reached the point where I was working twelve to fourteen hours every day, including weekends.
Due to the additional stress from work I strayed from my diet and became very ill. I had huge problems with my knees and this triggered inflammation in many other joints too.
Unfortunately I had to keep working on-site and away from my office and home, so I began to eat and drink things which I knew would cause problems, but at the same time I needed the energy and often the caffeine too :-)
Eventually I reached the point where I needed to have cortisone injections in my knees again, in order to continue working. I kept saying to myself, I will just get on top of things then go back to my diet and recover but new problems kept getting in the way.
The Original Cause of my Rheumatoid Arthritis – Discovered in Turkey!
As it happens, I recently went to Turkey to be with my mother-in-law (actually anneciğim in Turkish) because she was about to have a major operation. Unfortunately I was still ill myself and I became worse on the journey due to the flights, airports, taxis and such.
The first few days there I was very ill and had to go to hospital for treatment. While waiting for mum’s exact operation date to be confirmed, I also saw several other doctors myself regarding my RA (mostly friends of the family). This is where it got interesting!
I will write in more detail about my visit and the things I discovered there later, but in a nutshell; I discovered one of the original causes (possibly the only/main cause) of my rheumatoid arthritis :-)
The Turkish medical system is very flexible and responsive, and tests results & X-rays can be obtained almost immediately. As a result I was able to accumulate useful test results, scans and expert opinions in a very short timescale – just a few hours.
It was soon explained to me that I had a long standing blood infection that required urgent treatment; systemic inflammatory response syndrome – a kind of sepsis which can be fatal. My doctors there were amazed that I was still alive and equally amazed that I had managed to fly to Turkey in such a condition. They arranged for me to be admitted to hospital for treatment and monitoring and I started taking oral antibiotics soon after an initial intravenous injection.
After discussing the history of my symptoms and studying my many new test results they concluded that I had probably had this infection to some degree for at least the last twenty-five years, but that it was currently life threatening. If I had not gone to Turkey, I would perhaps never have realised the serious state of my disease and would have continued to believe that my symptoms were just a flare-up of my existing RA – and possibly died.
My RA Caused by Tooth Infection Missed by Doctors and Dentists
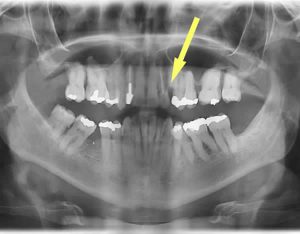
I was immediately given powerful antibiotics and then referred to a dental surgeon in a local specialist hospital (another family friend) as my doctors suspected a long standing tooth abscess was the original source of the infection. In our discussions, I explained that I had had a problem tooth for about thirty years and that it often caused pain, bad breath and various other symptoms. I also explained that I had brought it up with several of my UK GPs over the years but that they had always dismissed it as a possible cause of my RA and had not considered it to be a serious problem. Unfortunately, after several soul destroying attempts to obtain dental treatment in the UK, I eventually gave up and just accepted the pain. Had I known the extent of the problem, I would have persevered of course and obtained treatment, somehow.
The dental surgeon confirmed my doctors’ suspicions with the help of various scans, examinations and blood tests. Again, he could not believe the extent of the infection and explained that it was difficult for him to remove the problem tooth in my current condition as it was too badly infected. He prescribed additional specific antibiotics to complement the ones obtained from my doctors and asked me to call in periodically to monitor my progress. He also shared his findings with my doctors.
A few days into taking the antibiotics, my symptoms started to improve, particularly in my mouth of course but also I noticed a greater range of movement in some of my fingers and my feet were no longer swollen. A week later whilst discussing new blood test results with my doctors, they confirmed that I had achieved about a 30% improvement in the severity of my infection (apparently enough to silence the alarm bells). Following on from this, they advised me that it would take between one and three years of oral antibiotic treatment to completely clear the infection, along with appropriate dental treatment. My doctors also explained that intravenous antibiotic therapy would be more effective but since I was only there for a short time, it wasn’t really practical because I wouldn’t be able to continue the treatment in the UK.
The upshot of all this is, I have proof of what I always suspected to be the case; that my joint inflammation was caused (in part or wholly) by some type of infection, and now I know what it was and how it started; a streptococci group – tooth/gum infection which gradually became a hidden abscess inside my gum/jaw where most of the infected tooth broke away and left a deep hole which never healed.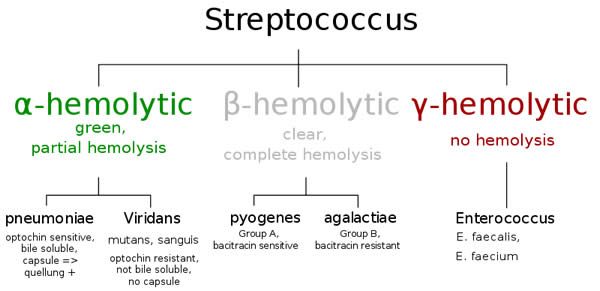 Streptococcus mutans causes plaque, tooth erosion and cavities and this was probably what initiated my problem decades ago. However, my systemic infection appears to have been caused by group A or B streptococcus originating either directly from my long-term tooth infection/abscess, or by external infection from some contaminated food or drink due to the susceptibility of my broken tooth and the deep surrounding abscess. Unfortunately, because of the rush to administer antibiotics and because I was feeling so ill, I never managed to obtain further more detailed tests to confirm exactly which strain caused or worsened my joint inflammation. However I suspect ‘pyogenes’ because of my symptoms; swollen lymph nodes, intermittent fever, increased joint inflammation, flu symptoms, skin rash etc.
Streptococcus mutans causes plaque, tooth erosion and cavities and this was probably what initiated my problem decades ago. However, my systemic infection appears to have been caused by group A or B streptococcus originating either directly from my long-term tooth infection/abscess, or by external infection from some contaminated food or drink due to the susceptibility of my broken tooth and the deep surrounding abscess. Unfortunately, because of the rush to administer antibiotics and because I was feeling so ill, I never managed to obtain further more detailed tests to confirm exactly which strain caused or worsened my joint inflammation. However I suspect ‘pyogenes’ because of my symptoms; swollen lymph nodes, intermittent fever, increased joint inflammation, flu symptoms, skin rash etc.
This of course makes me think that there could be many more people out there suffering with rheumatoid arthritis or other inflammatory conditions, who may have a tooth related infection (there appear to be three types of tooth/gum abscesses) and who may not realise its importance as a potential cause of their disease.
I want to recommend that if you have any kind of tooth decay/pain/abscess and also suffer from RA, get your teeth looked at and get any problems fixed straight away, even if like me you have been putting it off or putting up with it. Also, if you do a little research, you will quickly find a number of papers and articles like this one confirming the link between abscess infection and rheumatoid arthritis and this example of a link between a dental streptococcal infection and rheumatoid arthritis.
![]() “Streptococcus” image is public domain
“Streptococcus” image is public domain ![]()
Pull it Charlene pull it out that root filling nonsense. All of them! I can only recommend!
Hi Jacob, thanks very much for your comment.
I too have a problem with joint pain that seems to move from place to place on a daily basis, which started with an abscessed tooth. I since had a root canal and the tooth capped, but the tooth still bothers me. I spent 2 months on antibiotics and thought it was possibly the antibiotics causing the pain. My dentist sent me to a specialist in which he did another root canal and found I had a hairline crack in the tooth, which my dentist did not have the instrument to see at the time of the abscess. The specialist filled the crack the best he could and filled the tooth and new crown. Boy, was I upset for spending $900 on a crown that had to be drilled into. Anyway, the tooth still bothers me and I still have the joint pain. My next step is to have the tooth pulled. Hopefully this joint pain will go away once my body longer has an intruder of infection from this tooth from hell. This has been going on since last July. The joint pain can be so severe at times, I will not be able to walk. On a good note, I have been taking a tsp of baking soda once a day and seems to control the joint pain when I get it. Believe it or not, it works…
Hi Charlene, thanks for your comment.
I’m so sorry to hear that you had so many problems with your tooth/cap, I hope you managed to resolve the problem since you commented. It must have been very difficult to go through all that only to find that you had a hairline crack and had to deal with the issue all over again. Let us know how you got on since then. I’m glad the baking soda is helping you, there are a lot of reports of it helping with joint pain.
Hello I’m glad to hear your RA has subsided. Wouldn’t wish it on anyone! I’m curious as to the antibiotic treatment,what antibiotics how many different ones< how long did you take this? I have a bad tooth for how long I’m not sure. I will be getting it pulled soon, and hopefully on a antibiotic. Thanks for your story, I have been searching for a long time for something. My Rheumatologist unfortunately doesn’t buy into all of this. After tooth removal I will see how it helps and find someone how is on my side.
There is a documentary on Netflix called “Root Cause”. It is exactly about this situation. I highly recommend you watch it.
Hi Julie, just wanted to thank you for helping Paula :-)
Hi Paula, thanks for your comment.
I took doxycycline for a few weeks after being diagnosed with a form of sepsis caused by an infected tooth/gum. During that time my arthritis calmed down quite a bit, but I wouldn’t recommend antibiotics as a treatment. I also tried the Antibiotic Protocol which is a treatment protocol developed specifically for rheumatoid arthritis, but unfortunately it produced some serious side effects which is a shame because it did help with my arthritis symptoms, though again I wouldn’t recommend it as a treatment. However, there is no doubt in my mind that tooth/gum infection can be a cause of rheumatoid arthritis and/or a promoter of it. So having your infected tooth removed as an excellent idea. Good look with your treatment.
Hi, I have had RA seropositive, for 20 years and mostly mild, until recently. I have been vegetarian for more than 30 years. My current and most severe flare follows the death of my mother 2 yrs ago, early retirement and a move to Scotland to be closer to my son and his family. My RA began when my dad became terminally ill. Both my RF and Anti-CCP are high. Through a strict diet, I managed to come of Methotrexate, but my diet slipped substantially, when mum died and has not been great since. I am currently trying to get back to the original diet but struggling and am in my worst flare. I now need to go back to the strictest of anti-inflammatory diet, I know.
Could I ask what your RF and Anti-CCP levels are?
Do you take probiotics such as Kefir and have you studied this?
Thanks and good wishes Julia
Hi Julia, thanks for your comment sorry for my late reply, I’m really sorry to hear about your mother and then your father.
Severe stress can often make rheumatoid arthritis much worse and can even cause it in some cases, partly due to the link between the gut and the brain. I understand how difficult it is to stick to a strictly anti-inflammatory diet, I work hard each day to achieve this because I know it’s the only way to maintain recovery however slowly.
I haven’t had my rheumatoid factor or CCP levels checked for some time, but in the past when I fully adopted a whole food plant-based diet my rheumatoid factor, sedimentation rate and CRP began falling dramatically (I didn’t check my CCP). Yes, I take a broad range of probiotic bacteria and I eat foods such as raw miso and natto as well as lots and lots of high-fibre prebiotic foods.
Thanks very much Julia, my best wishes to you too XX
PS. We also introduced Serrapeptase a Protyolitic Enzyme that removes bacterial biofilm and un wanted protein in the body. My understanding is that Biofilm stops the antibiotic penetrating and killing the bacteria. So along with Stevia which has the same effect and multistrain Probitotics we have been able to beat this thing. His RA factor went from greater than 600 to 70 in March of this year. We will see Drs again in a couple of months and get some bloodwork done. My argument as an old RN is that the USA top ” normal” range of 10000 for white cell count is too high and is an indication of infection somewhere in the body.
Hi Geraldine, serrapeptase is an interesting enzyme, thanks for reminding me, I’ll study it further in the near future.
Probiotics can definitely help to reduce inflammation and improve gut health. I’m so happy to hear that his rheumatoid factor has fallen so dramatically! :-) I agree with you regarding the white cell count, in fact I believe a white cell count slightly below the ‘normal’ range is the healthiest.